The Importance of Addressing Gender and Social Inclusion Barriers: WI-HER Partners With USAID Regional Health Integration to Enhance Services in Eastern Uganda to Address HIV viral suppression rates
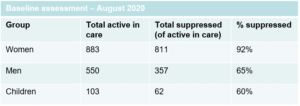
Since August 2020 – through the USAID Social Behavior Change Activity – WI-HER has been working closely with USAID Regional Health Integration to Enhance Services in Eastern Uganda (RHITES-East) Project and Tororo District’s Nagongera health center (HC) IV facility staff to address poor viral suppression rates (Table 1). HIV positive clients of Nagongera HC IV were missing appointments and not adhering to antiretroviral therapy (ART) required to achieve viral suppression.
To be virally suppressed means that a person can effectively no longer transmit HIV to another person and is thus critically important to ending the HIV epidemic. As seen in the table below, the largest gap in viral load suppression was in men and children. In close partnership with the USAID RHITES-East team, WI-HER applied its iDARE methodology to help Nagongera health facility staff identify gender and social inclusion barriers that contribute to lack of adherence and/or missed appointments, and to design local solutions to help people living with HIV to improve HIV and other health outcomes.

WI-HER supported the Nagongera facility and RHITES-East to conduct a rapid gender assessment to understand barriers, which led to the establishment of an iDARE team of people best able to implement agreed upon solutions to overcome identified barriers. The iDARE team is comprised of health facility staff and community influencers. The community influencers on the iDARE team were proposed by the HIV positive clients due to their trusted role in providing client-centered care.
iDARE team members established a small “cohort” of 14 men and 16 children who were not suppressed at baseline (August 2020). The team then started to address gender equity and social inclusion issues that impacted the cohort’s adherence (and or access) to treatment. Establishing a cohort is the first step to support all men and children who are actively enrolled in care at Nagongera HCIV to be virally suppressed. The iDARE team continuously engaged fellow community members on addressing identified gender-related barriers, and after two months of implementing solutions, the facility reported that 50% of the first cohort of men adhered to their scheduled clinic appointment. By early December, viral load suppression rates increased from 0% within the cohort to 71% for men and 50% for children. The improvements in viral load suppression contribute to the overall men and children viral load suppression rate from 65% and 60% (at baseline) to 67% and 68% (first week in December), respectively.
To highlight the incredible work of this dedicated group of community influencers and health workers, we requested several to share their experiences and testimonies of how addressing gender and social inclusion barriers at the community level leads to improved HIV and health outcomes.
- Pastor Henry’s thoughts on working on HIV at the Nagonga health center in Uganda.
- Achiya Michael’s thoughts on working on HIV at the Nagonga health center in Uganda.
- Olowo John’s thoughts on working on HIV at the Nagonga health center in Uganda
- Sister Annet Grace Naula’s thoughts on working in HIV at the Nagonga health center in Uganda